Endoscopic surgery is a minimally invasive procedure that has been commonly used in a wide range of applications. During endoscopy, rigid endoscopes are passed through small incisions or natural orifices to guide healthcare professionals in diagnostics and surgical interventions [1,2]. For this, good image quality is critical to distinguish between different tissue types [1,2].
As rigid endoscopes are too expensive to discard after each surgery, they go through reprocessing several times [3]. Reprocessing consists of monitoring the effectiveness of washer-disinfector cleaning. It uses biological and chemical indicators to detect contamination in packages sterilized in the autoclave, allowing reusing the device [4].
Also, the endoscope is a complex and fragile device that can easily damage during use. Starting surgery with defective equipment can increase the length of the procedure, lead to misdiagnosis and mistreatment due to poor image quality. Therefore, it is vital to maintain the endoscope's quality and functional characteristics after reprocessing [1,2].
The primary test performed to assess the endoscope's quality is a simple visual inspection. However, this visual assessment is challenging, and defects are often only detected in the operating room [1–3].
To address this issue, other measures can be handy.

ScopeControl®
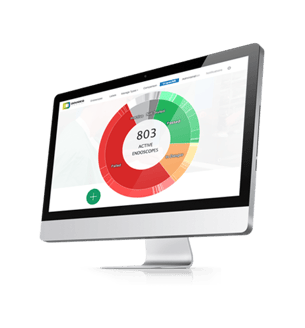
ScopeControl® controls the quality of rigid endoscopes to eliminate human errors and perform more in-depth analyses. The device ensures the optical quality of endoscopes in a clinical setting, with reliable reproducibility and accuracy [1]
How does it work?
ScopeControl® automatically measures the optical quality of an endoscope to determine if it is of sufficient quality for use [3].
It contains a high-definition camera that looks through the endoscope. It makes several captures and compares them with the device's parameters [3].
A value of 100% refers to the best-measured endoscope, and below this value, the performance is not so good. However, if the value falls below a threshold, it enters the red "zone," which means it is inappropriate and cannot be used in surgery [3].
EndoscopeManager
Healthcare leaders are increasingly improving the quality of care with highly professional practices and processes to meet patients' expectations [5].
Strict endoscope handling is necessary to ensure excellent and safe conduct in surgical procedures. The EndoscopeManager is a perfect ally for managing endoscope reprocessing logistics. This ScopeControl® extension allows checking for device defects remotely on a cloud platform.
In this way, you can correct problems as they are identified, reducing repair time and costs, and increasing the device's reliability. The platform also provides damage and repair reports for further monitoring of the maintenance process [5].

DoviSCAN
In September 2013, the FDA determined a rule to establish a Unique Device Identification (UDI) system. The goal was to improve after-sales surveillance, device tracking, and data integration into patient health records [6].
A UDI is an alphanumeric code that works like a bar code and is unique for each specific medical device. This code is essential to standardize the labeling and identification of equipment and facilitate its monitoring.
To ensure the safe reading of IDUs on medical instruments, DoviSCAN, a data matrix scanner, is equipped with BlueLed technology to read small 2D matrix codes. It is a compact, resistant, intelligent device suitable for medical use and can be connected directly to the USB port.
Consequently, standardization and ease of reading IDUs, generate efficiency in care, directly impacting the patient's well-being, allowing more accessible and accurate information about medical devices [6].
Conclusion
Endoscopy is a relatively simple and highly used procedure. For high reliability, you must be ensured that the image is of good quality.
Because they are fragile equipment, endoscopes must be handled with care, especially during reprocessing.
These processes can be automated to allow better reproducibility and reduced costs.
References
- 1) Courault P, Emery S, Boudour S, Rochefort F, Ruffion A, Dussart C, et al. Quality control of rigid endoscopes: a comparative study between ScopeControl® and surgeons' evaluation. Surg Endosc. 2021. doi:10.1007/s00464-020-08181-4
- 2) Wientjes R, Noordmans HJ, Eijk JAJ va. der, Brink H van den. Automated Objective Routine Examination of Optical Quality of Rigid Endoscopes in a Clinical Setting. PLoS One. 2013;8: 1–7. doi:10.1371/journal.pone.0059579
- 3) Noordmans HJ, de Braak M, Wientjes R, Martens E, Lindenhovius K, Swart P. Evaluation of the ScopeControl endoscope test system in six hospitals in The Netherlands. Phys Medica. 2015;31: 152–158. doi:10.1016/j.ejmp.2014.12.006
- 4) Alfa MJ. Quality Systems Approach for Endoscope Reprocessing: You Don't Know What You Don't Know! Gastrointest Endosc Clin N Am. 2020;30: 693–709. doi:10.1016/j.giec.2020.06.005
- 5) Armellino D. Ongoing discovery of high-level disinfection of endoscope practices and the use of performance improvement methodologies to improve processes. Jt Comm J Qual Patient Saf. 2016;42: 262–264. doi:10.1016/S1553-7250(16)42034-9
- 6) Brown C, Kaushiva A. Incorporating unique device identification into your hospital. J Clin Eng. 2015;40: 87–89. doi:10.1097/JCE.0000000000000090